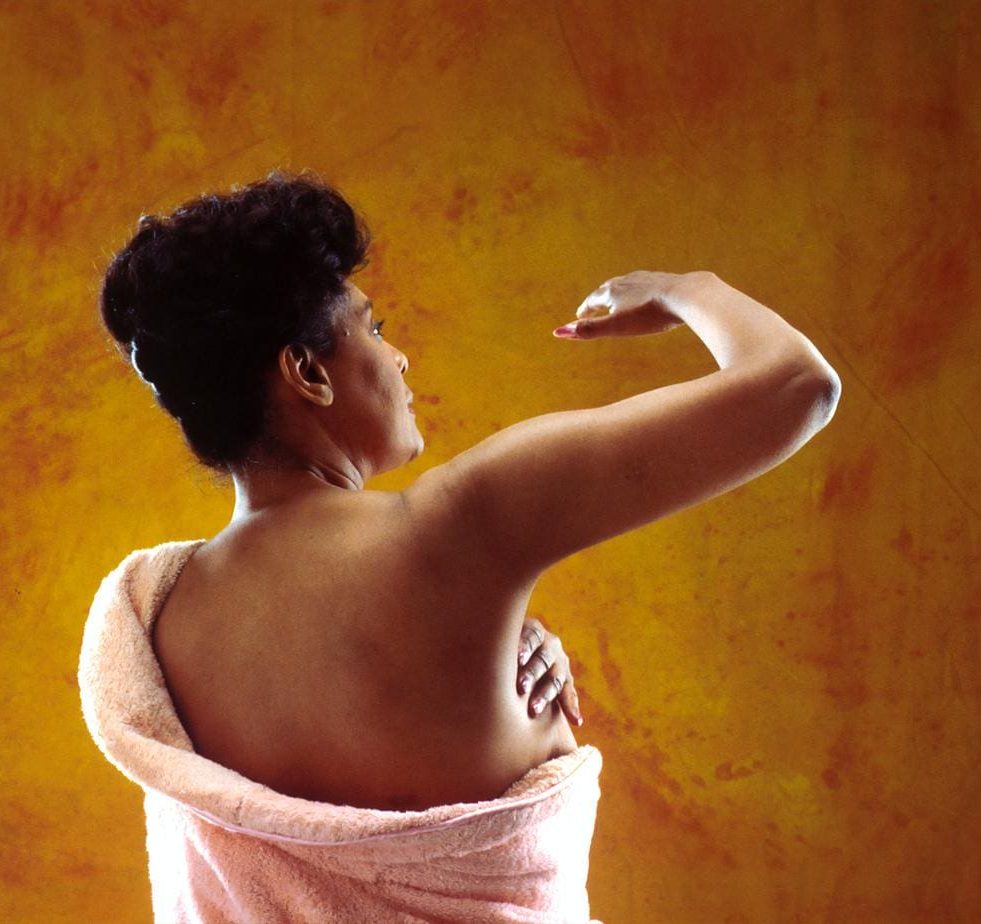Editor’s Note: The information contained in this article is not gender specific, and is intended to be helpful across all gender identities. We predominantly use the word “breast” in this article, as that is the terminology most commonly used to refer to these types of cancers.
Whilst all the links are recommended by the author as sources of information, they may be limited in how they address gender beyond the binary. We would like our trans, intersex and nonbinary readers to be aware before following any of these links.
Breast Cancer Stats
Breast cancer is the most common type of cancer in the UK. There are nearly 56,000 British diagnoses of Breast cancer every year. 1 in 8 people develop breast cancer at some stage in their lifetime, and 1 in 5 of these will be under 50.
According to Breast Cancer Now, breast cancer affects mainly cis-gender* women over 50, with this demographic making up 80% of cases. “The older you are, the higher your risk,” they state.
And, of course, men of any gender identity can also get breast cancer. The incidences for breast cancer in this demographic are far lower, with less than 1% of breast cancer occurring in men. Most men who get breast cancer are over 60.
* cis-gender means people whose gender identity aligns with their sex assigned at birth.
How To Check Your Breasts
How often should I check?
Checking your breasts, chest and armpits (these are all areas that can exhibit early signs of abnormalities) could help you spot the symptoms of cancer early on and genuinely could save your life.
It’s essential that you schedule at least one check every month or so.
Breast Cancer awareness charity CoppaFeel have a huge amount of useful resources on their site, including their Self-Checkout (which you can personalise to use the language that feels right for you), which offers reminders to check as well as stickers and guides on how to check yourself.
Help to raise awareness with friends and family (remember, of any gender!) and remind them to check regularly too.
How do I check?
It’s important to know what your body usually looks and feels like so you can recognise when something has changed. If you do notice any changes, you’ll be able to report it to your GP more accurately, which may help with a speedy diagnosis and treatment.
Editor’s note If you find it particularly difficult to look at, photograph, or feel over this area of your body due to gender dysphoria, you may want to access help and support from an organisation such as the Terence Higgins Trust.
One way you can get to know yourself is by taking topless selfies! You can save these to a private photo album on your phone, or a password protected folder on your laptop. You also wouldn’t need to have your face in these images, so they can be relatively anonymous.
Taking photos can help you to document the shape, size, and presence of any visible lumps and bumps. Take a photo once a month when you do a thorough check, and you’ll soon have a good visual guide to any changes. These photos are not meant to be tastefully candle-lit nudes, either. Work with good light so you can really see if there are any changes of note.
You can also do a quick check every time you have a bath or shower. Just run a soapy hand over your chest, breasts and under each armpit to feel for anything new.
These quick feels don’t replace the more detailed monthly checking, but again they can help to familiarise you with your body and make you aware of any new changes.
You can also look at your body in the mirror, if that is something you feel able to do.
Facing yourself in the mirror, alternate between two positions to spot any irregularities:
- With your arms by your side
- With your arms raised
Lumps are vital to look out for, but, more often than not, they are benign. There are other vital signs and symptoms to check for too, such as changes in skin texture, discharge from the nipple and swelling in the armpit or around the collar-bone.
What should my breasts look and feel like?
Every person’s breasts are different.
The size, shapes, and consistency will alter from person to person. An individual person’s breasts can change for all sorts of reasons, through changes at puberty, taking hormonal contraception, pregnancy, breast-feeding, menopause and growing older.
It’s also pretty standard for one breast to be bigger than the other. 1 in 4 people have some degree of asymmetrical breasts.
This doesn’t mean, for one second, that there’s anything wrong with them.
The key is in knowing your body. If your breasts were totally symmetrical a few months ago and they’re now noticeably different sizes, it’s best to get checked.
Your breasts can also feel different at varying times of the month, especially (but not only!) if you are someone with a menstrual cycle.
During this time, breasts can become tender and lumpy, especially around the armpit. Breasts can also become itchy, sore or lumpy during ovulation. So, if someone experiences from breast pain and/or lumps during ovulation and menstruation, that only leaves an average of two weeks per month where the body is settled again. This is why documenting any changes can help you to spot if there is a pattern (always lumpy and sore around menstruation, for example), and to notice when there is a deviation from that pattern.
What to check for when checking your breasts
The NHS website lists things you should be looking and feeling for when you check your boobs:
🍊a change in the size, outline, or shape of your breast
🍊changes in the look or feel of your skin, such as puckering or dimpling
🍊a new lump, thickening or bumpy area in one breast or armpit that is different from the same area on the other side
🍊nipple discharge that’s not milky (if you’re not lactating, it’s worth getting any discharge checked out by a doctor)
🍊bleeding from your nipple
🍊a moist, red area on your nipple that doesn’t heal easily
🍊any change in nipple position, such as your nipple being pulled in or pointing differently
🍊a rash on or around your nipple
🍊any discomfort or pain in one breast, particularly if it’s a new pain and doesn’t go away (although pain is only a symptom of breast cancer in rare cases)
Do breast implants cause breast cancer?
There is no link suggesting that having breast implants will increase your chances of getting breast cancer.
If you’re considering any kind of breast surgery, but you’re concerned about breast cancer, you can discuss this in-depth with your surgeon at your consultation.
You will need to refamiliarise yourself with your body after any chest or breast surgeries, to get used to your new normal.
Risk factors for breast cancer
There are many risk factors for breast cancer.
However, it’s important to note that you may never get breast cancer even if you have all of these risk factors. Similarly, you could have none of these risk factors and still develop breast cancer.
Some risk factors for breast cancer that you can control are:
- Radiation exposure
- Obesity or being overweight. Being overweight means having a body mass index (BMI) of between 25 and 30. Obesity means being very overweight with a BMI of 30 or higher.
- Drinking alcohol – if you need help reducing your alcohol intake, follow this link to get advice from DrinkAware.
- Smoking – if you need help quitting the NHS has advice here.
However, risk factors for breast cancer that are out of your control are:
- Being assigned female at birth – although remember, people of all genders can develop breast cancer
- Getting older
- Having family members who had breast cancer
- Starting your period at a younger age
- Starting your menopause at a younger age
- Never carrying a child
Mammograms & Breast Screening
People in the United Kingdom aged 50+ are entitled to free breast screening, also known as a mammogram. These can still be done if you have breast implants.
You should get your first appointment between your 50th and 53rd birthday.
You’ll then receive invitations every three years until you reach 70.
If you don’t get an invitation to your breast screening book an appointment to discuss it with your GP.
If there is a history of breast cancer within your family, it may be that you have inherited a genetic predisposition. Being a carrier of these genes could increase your chances of developing breast cancer, but it is not a certainty. Most breast cancers happen by chance and only about 3% are due to an inherited gene.
If someone in your family has a history of breast cancer, you should discuss this with your GP. If your doctor considers you to be at risk because of your family history, they may recommend genetic testing or earlier screenings.
Early detection really could save your life.
So get to know your body, have a good look and feel, and show yourself some love.
For more information on breast cancer, please visit Breast Cancer Care or Cancer Research.
Still have questions about how to check your boobs for lumps and bumps? Make sure you check out the fantastic CoppaFeel website.
Global Breast Cancer Resources For Patients, Survivors and their Loved Ones
A truly comprehensive list: whether you’re looking for companies that support breast cancer awareness, places to donate or products for people with breast cancer, you will find what you’re looking for here.

Written by the Killing Kittens team.